Time-based, modifier-intensive anesthesia revenue cycle management designed to maximize reimbursement and ensure full CMS compliance.
Maryland-Based Medical Billing Company | Serving Practices Nationwide | Hospitals, ASCs, Office-Based & Pain Centers | HIPAA-Compliant & CMS-Aligned
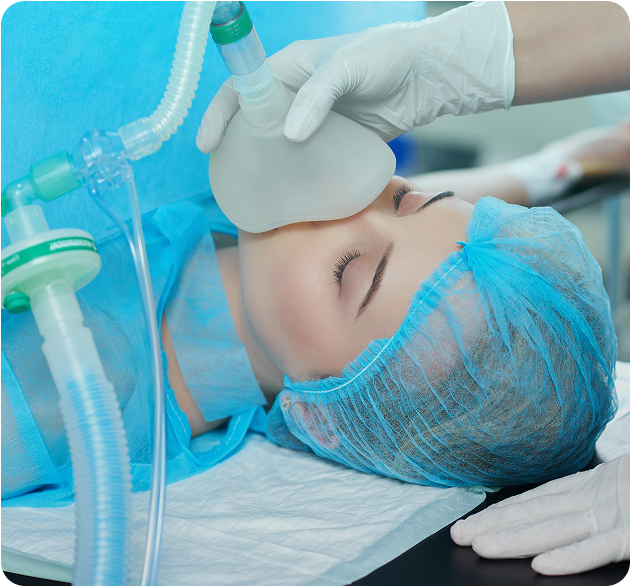
Anesthesia billing is fundamentally different from general medical billing. Unlike standard CPT-based services, anesthesia reimbursement is time-based, with payments calculated from a combination of base units, time units, and modifiers. Each minute of anesthesia must be documented precisely, and rounding errors or missing time entries can lead to rejected or underpaid claims.
Concurrency restrictions further complicate billing. For instance, CRNAs and anesthesiologists can only supervise a limited number of cases simultaneously, and exceeding these limits can result in denials from Medicare and commercial payers. Proper documentation of medical direction or supervision is critical to ensure compliance.
Anesthesia practices face higher denial rates than most specialties, partly due to the complexity of modifier usage and time-based calculations. Medicare closely scrutinizes anesthesia claims for accuracy in time units, physical status modifiers (P1–P6), and medical direction modifiers (AA, QK, QX, QY, AD). Even small mistakes can result in lost revenue or audit exposure.
The Centers for Medicare & Medicaid Services (CMS) and the American Society of Anesthesiologists (ASA) provide detailed guidance on coding, time calculation, and modifiers. Navigating these regulations requires specialized knowledge and constant updates.
As a full-service Maryland medical billing company, Medhasty brings deep, anesthesia-specific expertise to every practice. Our team ensures clean claims, accurate modifier application, and fully documented time-based billing, reducing denials and maximizing reimbursement across all settings—from hospitals and ASCs to office-based and pain management practices.
CPT codes 00100–01999 are carefully reviewed for accuracy, with ASA crosswalks validated and modifier stacking checked to prevent errors before claims are submitted.

Start and stop times are audited, rounding compliance verified, and concurrency limits for CRNAs and teaching anesthesiologists are closely monitored to avoid denials.
Claims are submitted for hospital-based anesthesia, ambulatory surgery centers, office-based anesthesia, and pain management procedures, ensuring complete coverage across every care setting.
Denied claims due to time unit disputes, modifier errors, or medical necessity issues are investigated, corrected, and appealed to recover lost revenue efficiently.
Clean claim rates are monitored, days in AR are tracked, conversion factors are audited, and revenue leakage is identified to provide full-cycle visibility and actionable insights.
Workflows are tailored for Medicare, Medicaid, commercial payers, workers’ compensation, and out-of-network claims to maximize reimbursement and reduce delays.
We handle:
Medhasty is a full-service anesthesia billing company that understands the nuances of cross-specialty billing.
Anesthesia billing is layered and high-risk. Diagnostic testing, chronic disease management, infusion therapy, and strict payer oversight create constant pressure on revenue cycle teams. Below are the most common challenges neurologists, practice managers, and revenue cycle directors encounter:
CRNA Billing & Supervision Rules: Accurate claims for independently billing CRNAs and those under supervision.
Medical Direction vs Medical Supervision: Differentiating roles and applying correct modifiers to avoid denials.
Monitored Anesthesia Care (MAC) Billing: Time, base units, and modifiers are audited to prevent underpayment.
Teaching Anesthesiologist Billing: Concurrency, time reporting, and teaching involvement are tracked precisely.
High-Risk & Emergency Procedures: Emergency anesthesia is billed with full documentation to support increased units and modifiers.




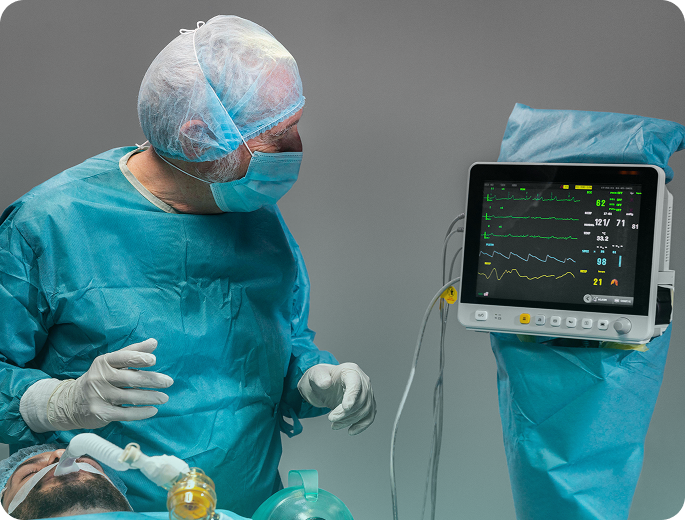
Medhasty ensures your anesthesia practice stays audit-ready and compliant with all Medicare anesthesia billing rules. Our team reviews medical direction documentation requirements, verifies the presence of a teaching anesthesiologist, and monitors concurrency limits to prevent audit risks. Proper start and stop time stamping is enforced, ensuring anesthesia time units are accurately recorded and defensible. We identify OIG audit triggers and guide modifier usage, including AA, QK, and QX, as well as medical direction billing nuances, so your claims meet federal and payer standards. By combining deep knowledge of anesthesia coding services, CRNA billing services, and ASA crosswalk validation, we proactively prevent errors that often lead to denials or repayment demands. Medhasty’s compliance-first approach protects your revenue, reduces exposure to penalties, and ensures every hospital, ASC, or office-based anesthesia claim is submitted confidently.
Medhasty is a Maryland-based medical billing company combining local accountability with nationwide expertise in anesthesia billing services. From our offices in Baltimore, Annapolis, Columbia, and Rockville, we serve anesthesiologists, CRNAs, and anesthesia groups across all 50 states, ensuring every claim complies with Medicare anesthesia billing rules and commercial payer requirements. Our team applies deep knowledge of anesthesia revenue cycle management, ASA crosswalks, time-based billing, and modifier usage to optimize reimbursement for hospital-based anesthesia, ASCs, office-based anesthesia, and pain management procedures. By blending local insight with national payer familiarity, Medhasty delivers accurate, compliant, and timely billing solutions that reduce denials, accelerate collections, and protect your anesthesia practice from audits.

Formula: (Base Units + Time Units + Modifying Units) × Conversion Factor
Base Units and the ASA Relative Value Guide
Each procedure has a defined base unit value, referenced from the ASA Relative Value Guide. Correct application is essential to prevent underbilling.
Time Units and Start/Stop Documentation Requirements
Time-based reimbursement depends on accurately recorded start and stop times. Proper documentation prevents rounding errors and ensures compliance with CMS guidelines.
Physical Status Modifiers (P1–P6)
Modifiers P1–P6 capture patient health status and influence reimbursement. Misapplication can trigger denials and compliance risks.
Medical Direction Modifiers (AA, QK, QX, QY, AD)
Modifiers define the provider role and supervision level. Accurate use avoids rejected claims and ensures CRNA and anesthesiologist billing alignment.
Stop leaving revenue on the table due to time calculation errors, modifier mistakes, and payer compliance gaps. Medhasty delivers expert anesthesia coding services, clean claims submission, and comprehensive anesthesia revenue cycle management across hospitals, ASCs, office-based practices, and pain centers.
Our solutions include:
Free Anesthesia Billing Audit to identify revenue gaps
Revenue Gap Analysis for lost or underpaid claims
Strategy Consultation to optimize workflows and compliance
Compliance Risk Assessment aligned with CMS, OIG, and ASA guidelines
FAQS
Anesthesia billing relies on time-based reimbursement, physical status modifiers (P1–P6), and medical direction rules, unlike standard CPT-based claims. Proper documentation, ASA crosswalks, and concurrency tracking are critical to ensure accurate payments and avoid denials under Medicare anesthesia billing rules.
Time units are derived from documented start and stop times for each anesthesia session. Rounding rules, concurrent case monitoring, and validation of teaching anesthesiologist presence are essential to maintain compliance and maximize reimbursement for both hospital and ASC services.
Medicare conversion factors differ by region and year, directly impacting reimbursement for base and time units. Applying the correct conversion factor ensures each claim reflects accurate compensation under Medicare anesthesia billing rules.
These modifiers specify the provider's role, including medical direction or supervision of CRNAs. Correct use is vital for documenting responsibilities and aligning with CMS concurrency regulations to prevent payment denials.
Per CMS rules, anesthesiologists may supervise a maximum of 1:2 cases for CRNAs and 1:4 for teaching anesthesiologists. Exceeding these limits can trigger denials and OIG audit scrutiny, underscoring the importance of anesthesia revenue cycle management oversight.
Records must confirm anesthesiologist involvement, including pre-anesthesia assessment, intraoperative oversight, and total time spent supervising CRNAs or Monitored Anesthesia Care (MAC). Accurate documentation supports modifier application and audit protection.
Common denials arise from incorrect time unit calculations, missing or misused modifiers, inadequate documentation, exceeding concurrency limits, or misapplied conversion factors. Proactive denial management and appeals minimize lost revenue.
Certified Registered Nurse Anesthetists (CRNAs) may bill independently for anesthesia services in states and settings where allowed. Independent billing requires strict documentation of start/stop times, procedures performed, and modifier application (such as QZ for unsupervised CRNA services). CMS and commercial payers monitor compliance with medical direction billing rules, so accurate records and expertise in anesthesia coding are essential to prevent claim denials.
Accounts receivable (AR) for anesthesia claims vary by payer, setting, and documentation quality. Hospital and ASC claims typically post within 30–45 days when clean claim submission and time unit validation are followed. Denied or incomplete claims can extend AR to 60–90 days or longer. Proactive anesthesia denial management, regular follow-up, and detailed revenue analytics reduce turnaround time and accelerate cash flow for anesthesiologists, CRNAs, and anesthesia groups.
Let our medical billing experts optimize your revenue cycle management. We enable healthcare practices to increase cash flow and avoid denials. Permanently!