Medhasty provides specialized ENT billing and revenue cycle management services for otolaryngology clinics across the United States. Our billing specialists manage ENT procedure coding, surgical billing, and payer compliance to help practices reduce denials and accelerate reimbursement.
ENT practices face billing complexities that differ significantly from many other medical specialties. Otolaryngology visits often involve diagnostic testing, minor procedures, and surgical interventions performed during the same encounter. Without accurate coding and structured billing workflows, these complexities can lead to claim denials, delayed reimbursements, and administrative burden for clinic staff.
Multiple Procedures During a Single Encounter: ENT appointments frequently include diagnostic exams, procedures, and treatments performed during the same visit. Procedures such as nasal endoscopy, audiology testing, and minor surgical interventions require precise coding and appropriate modifier usage to prevent bundled claim denials.
Modifier Complexity in ENT Billing: ENT billing often requires correct application of modifiers such as Modifier 25, Modifier 59, and Modifier 50 to indicate separate services or bilateral procedures. Incorrect modifier usage is one of the most common causes of claim rejections in otolaryngology billing.
Surgical Global Period Management: Many ENT procedures including septoplasty, sinus surgery, and tonsillectomy are subject to global surgical periods. These billing rules require careful management of pre-operative and post-operative services to ensure claims comply with CMS guidelines.
Prior Authorization Requirements: Certain ENT procedures such as balloon sinuplasty and sleep apnea surgeries require prior authorization from insurance providers. Failure to obtain authorization before treatment may result in denied claims.
ENT specialists perform a wide range of diagnostic and surgical procedures that require accurate CPT coding and clinical documentation. Medhasty’s billing specialists are experienced in coding and billing for procedures commonly performed in otolaryngology practices.
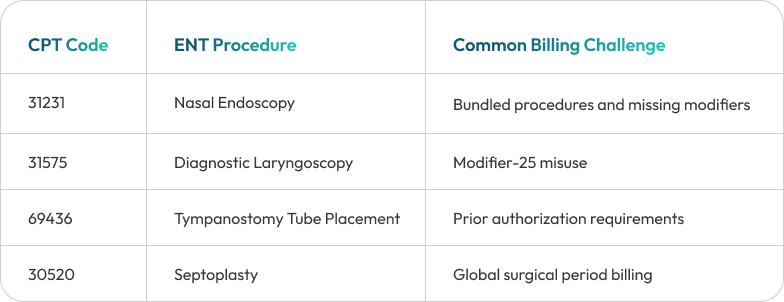
Procedures such as nasal endoscopy and tympanostomy tube placement represent a significant portion of outpatient ENT billing volume. Accurate coding and modifier usage are essential to ensure proper reimbursement.
Medhasty supports a wide range of otolaryngology practice models across the United States.
We work with:
Our billing workflows are customized to each clinic’s operational structure and payer mix.
Medhasty provides full-service revenue cycle management designed specifically for otolaryngology practices.
We confirm insurance coverage, benefits, and authorization requirements before services are performed.

Our certified coders assign accurate CPT, ICD-10-CM, and HCPCS codes for ENT procedures and diagnoses.
Claims undergo multi-layer validation checks before submission to ensure compliance with CMS and payer billing guidelines.
Denied claims are analyzed, corrected, and resubmitted with supporting documentation.
Insurance payments are posted accurately and compared against contracted reimbursement rates.
Our billing team actively follows up with insurance companies to ensure timely reimbursement.
Otolaryngology practices perform many surgical procedures that require careful billing coordination and documentation. Medhasty supports billing for procedures including:
Tonsillectomy and adenoidectomy
Myringotomy with tympanostomy tube placement
Tympanoplasty and mastoidectomy
Cochlear implant procedures
Vestibular function testing
Sleep apnea surgical procedures
Head and neck oncology surgeries

ENT billing must comply with regulatory and clinical standards established by organizations including:
Centers for Medicare & Medicaid Services (CMS)
National Correct Coding Initiative (NCCI)
HIPAA regulations
American Academy of Otolaryngology – Head and Neck Surgery (AAO-HNS)
Our billing processes ensure claims follow payer guidelines and documentation standards to minimize compliance risks.
Correct diagnosis coding ensures medical necessity for ENT procedures and reduces claim denials.

These diagnostic codes frequently accompany ENT procedure claims submitted to Medicare and commercial insurance providers.


ENT billing frequently requires modifier usage when multiple procedures are performed during the same visit or when bilateral anatomical structures are treated.
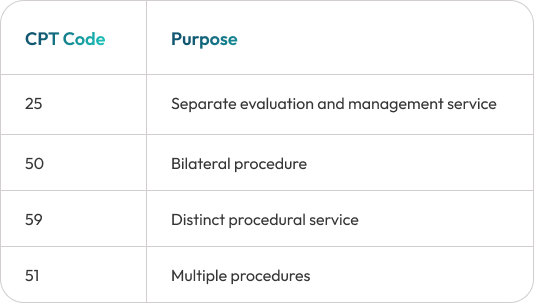
Proper modifier usage helps ensure ENT claims are processed accurately and reduces claim denial risk.
Managing ENT billing internally can overwhelm clinic staff due to the complexity of surgical procedures, diagnostic services, and payer requirements.
Medhasty’s specialized ENT billing services help otolaryngology practices:
reduce claim denials
improve clean claim rates
accelerate reimbursements
gain visibility into revenue cycle performance
FAQS
ENT billing involves complex procedures, surgical services, and diagnostic testing that require specialty-specific coding and documentation.
Yes. Our team manages billing for both office-based procedures and surgeries performed in hospitals or ambulatory surgery centers.
We use accurate coding, claim scrubbing, eligibility verification, and proactive denial management to improve claim acceptance rates.
Let our medical billing experts optimize your revenue cycle management. We enable healthcare practices to increase cash flow and avoid denials. Permanently!